A vaccine to prevent cocaine abuse proved mildly effective in its first placebo-controlled test. Although their individual responses varied, vaccine recipients reduced their cocaine use more quickly than placebo recipients. A subgroup of vaccinated patients generated levels of antibodies that were sufficient to block cocaine's effects, and during the period of peak antibody production, they submitted more drug-free urine samples than participants in the placebo group or those who did not respond strongly to the vaccine. With further refinement to increase response, a vaccine might someday be available as a therapy for cocaine abuse, says lead investigator Dr. Thomas Kosten of Baylor College of Medicine in Houston.
Testing the Concept
The cocaine vaccine consists of a small amount of the drug chemically bonded to a protein, derived from cholera toxin, that stimulates the immune system to produce antibodies (see illustration). Anti-cocaine antibodies latch onto cocaine molecules in the bloodstream, forming drug-antibody complexes that are too large to pass through the fine-grained tissue filter that enwraps and protects the brain. If the vaccinated person develops enough antibodies to capture and hold onto most of the cocaine molecules circulating in the blood, the drug will not produce the euphoria or other psychoactive effects that reinforce drug taking and addiction.
For the first placebo-controlled test of the vaccine's ability to reduce cocaine use among people who are addicted to the drug, Dr. Kosten and colleagues recruited 115 men and women who were seeking treatment at an outpatient clinic after having abused cocaine for about 15 years. The study participants were taking cocaine, on average, three times daily, 3 days per week. All were also addicted to opioids and had initiated methadone maintenance therapy 2 weeks prior to their first dose of the cocaine vaccine or placebo. The researchers chose this population because the patients came to the clinic daily to receive their doses of methadone, thereby increasing the likelihood that they would be available for injections, as well as urine and blood tests, and would remain in the study for its full 24-week duration.
Dr. Kosten and colleagues randomly assigned 58 patients to receive the cocaine vaccine in five intramuscular injections spaced over 12 weeks, a regimen that previous research had suggested should cumulatively produce enough antibodies to neutralize the amount of drug typically in the body during cocaine abuse. The remaining 57 patients received placebo injections on an identical schedule. All patients also attended weekly drug abuse counseling sessions focused on relapse prevention. The participants submitted urine samples for cocaine assay three times each week and gave blood samples for antibody level monitoring at the end of the second week and then at 4-week intervals.
Antibody Level Crucial
Some of the patients noted that the vaccine achieved its desired effect of suppressing cocaine's psychoactive effects. These individuals said that they felt little difference even after taking large amounts of the drug—in some cases up to 10 times their normal intake—confirmed by levels of a cocaine metabolite in their urine. In most of these cases, loss of cocaine's psychoactive effects occurred after three to four injections of the vaccine.
The patients who received the vaccine and those given placebo both reduced their cocaine use, but the former did so more rapidly. During the period of highest antibody response to the vaccine—from the week following the fourth booster injection through the month following the final one—30 percent of the vaccinated patients, but only 15 percent of the placebo patients, achieved a 50 percent reduction in cocaine-positive urine samples compared with levels at the beginning of the study. In prior research, this measure of success corresponded with improvements in daily functioning among people addicted to cocaine, Dr. Kosten says. No further injections were given after the 12th week of the study, and the difference in cocaine use between the vaccine and placebo groups disappeared by week 16.
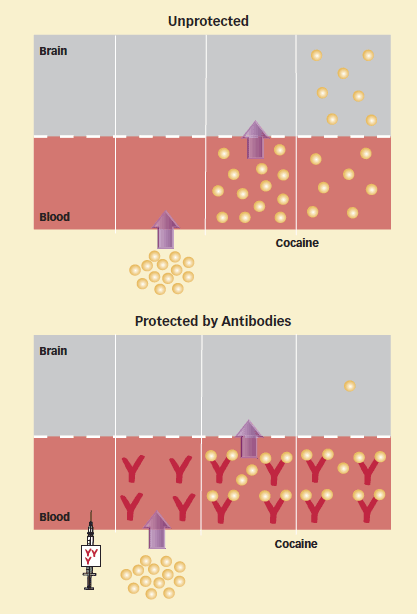 Vaccine Designed to Keep Cocaine Out of the Brain: Under normal conditions, cocaine molecules (shown as gold circles) easily cross from the blood into the brain (top diagram). A series of vaccines, however, stimulates patients' immune systems to produce cocaine antibodies (red Ys) that attach to molecules of the drug and prevent them from reaching the brain (bottom diagram).
Vaccine Designed to Keep Cocaine Out of the Brain: Under normal conditions, cocaine molecules (shown as gold circles) easily cross from the blood into the brain (top diagram). A series of vaccines, however, stimulates patients' immune systems to produce cocaine antibodies (red Ys) that attach to molecules of the drug and prevent them from reaching the brain (bottom diagram).The vaccinated patients varied greatly in their antibody responses, and only 38 percent of the 55 who completed the entire series of injections produced anti-cocaine antibodies in the quantity (at least 43 mg/mL of blood) that the researchers calculate will reliably block drug-induced euphoria. During the 8 weeks of the greatest antibody response, this group provided cocaine-free urine samples 45 percent of the time, as compared with 35 percent for the placebo group and the group with a lesser response to the vaccine. Of the patients who produced euphoria-blocking antibody levels, 53 percent at least doubled the frequency with which their urine samples demonstrated no new cocaine use, compared with 23 percent of those who received the vaccine but produced lower levels of the antibodies.
"If a patient makes enough antibodies, this treatment works well," says Dr. Kosten. Among cocaine abusers who receive the full course of injections, those who are motivated to quit are expected to achieve abstinence with a lower level of antibody than those who are not motivated to quit, he adds. Dr. Kosten estimates that, with the current vaccine, about 70 percent of cocaine abusers would develop high enough levels of antibody to block cocaine's euphoric effects by more than 90 percent, an effect considered sufficient to prevent relapse in individuals motivated to quit. However, people not motivated to quit but who receive the antibody treatment, perhaps in response to family pressure or other reasons, would require an antibody level high enough to completely prevent euphoric effects from whatever amount of cocaine they typically take.
There were no serious adverse events related to the vaccine, and no patients dropped out of the study because of the treatment. "The active protein components of this vaccine (cholera toxin B) and the adjuvant of aluminum are used widely; millions of people have received them," says Dr. Kosten. "Because the amount of cocaine in this vaccine is very small, it poses no threat to safety."
Improving the Vaccine
Dr. Kosten's team is currently planning to enroll 300 participants in a large NIDA-supported multisite trial to confirm the results of this proof-of-concept study and determine whether the vaccine can benefit the general population of cocaine abusers. The team expects the challenge of retaining patients for the entire course of vaccinations and assessments to be greater than in the just-completed trial, however, as none will be opiate abusers scheduled for daily clinic visits for methadone. To bolster participants' motivation, the researchers are supplementing relapse-prevention behavioral therapy with the opportunity to earn rewards for keeping clinic appointments.
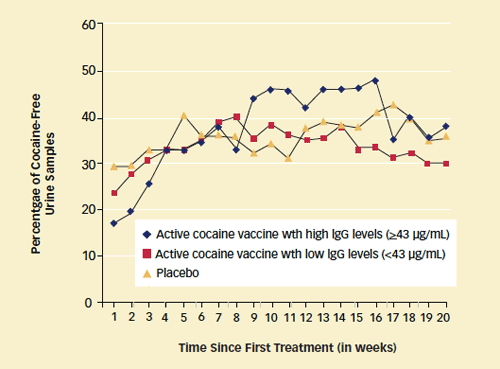 Antibodies Help Cut Cocaine Abuse: As the study progressed from week 1 to week 16, all patients reduced cocaine abuse—but vaccine recipients did so more quickly and to a greater extent. During the vaccination period, those who produced high levels of cocaine-blocking immunoglobulin G (IgG) antibodies (greater than or equal to 43 μg/mL) submitted a greater percentage of cocaine-free urine samples than participants who had a lesser response to the vaccine or those in the placebo group.
Antibodies Help Cut Cocaine Abuse: As the study progressed from week 1 to week 16, all patients reduced cocaine abuse—but vaccine recipients did so more quickly and to a greater extent. During the vaccination period, those who produced high levels of cocaine-blocking immunoglobulin G (IgG) antibodies (greater than or equal to 43 μg/mL) submitted a greater percentage of cocaine-free urine samples than participants who had a lesser response to the vaccine or those in the placebo group.In other ongoing research with different collaborators, Dr. Kosten is modifying the vaccine in hopes of producing a stronger, more sustained antibody response. The researchers have replaced the cholera toxin with a carrier molecule developed by Merck Pharmaceuticals from the Neisseria meningitidis bacteria coat protein, which has boosted the amount of antibodies produced by other vaccines. This carrier has been used in a human meningitis vaccine for over 10 years. The newly configured vaccine has reduced cocaine self-administration in animals but has yet to be tried in people.
Dr. Kosten envisions a 2-year course of vaccine-aided therapy for cocaine addiction that will include behavioral therapy and a series of vaccine injections followed by bimonthly or quarterly boosters.
Dr. Jamie Biswas of NIDA's Division of Pharmacotherapies and Medical Consequences of Drug Abuse agrees with this proposed length of treatment: "Patients need a couple of years of blocking the cocaine high to get used to being off the drug, and they may benefit from appropriate behavioral therapies as well.
"NIDA is interested in vaccines as a therapeutic strategy for mopping up an abused drug before it reaches the brain, as an alternative to addiction medications that influence the nervous system directly," Dr. Biswas adds. In addition to the cocaine vaccine, NIDA's immunotherapy program supports the development and testing of vaccines for smoking cessation and to counter overdoses of phencyclidine (PCP), methamphetamine, and amphetamine (see "Antibody Fragment Removes Methamphetamine From the Brain").
Source
Martell, B.A., et al. Cocaine vaccine for the treatment of cocaine dependence in methadone-maintained patients: A randomized double-blind placebo-controlled efficacy trial. Archives of General Psychiatry 66(10):1116–1123, 2009. [Full Text (PDF, 1.1MB)]