For many drug abuse patients, mood disorders are a constant companion. Among cocaine abusers, for example, depressive disorders are the most commonly diagnosed coexisting, or comorbid, conditions. The relationship between mood disorders and drug abuse in these patients is often complex and interconnected: Drug abuse patients may develop depression as a result of the physical and psychological suffering associated with their drug use, and patients suffering from mood disorders may become drug dependent in attempts to self-medicate. For patients suffering from both drug abuse and mood disorders, the conditions once seemed impossible to untangle, but recent NIDA research suggests that treatment for the mood disorder alone also can have a positive effect on drug abuse treatment.
One NIDA-supported study found that drug use declined among teenage drug dependence patients being treated with a medication for bipolar disorder, which is characterized by alternating periods of depression and mania. In a related study, chronic opiate-dependent adults reported less drug abuse when they were treated with the antidepressant imipramine for comorbid depression.
Reducing Substance Dependence in Bipolar Teens
Lithium has proven effective in treating adult bipolar disorder patients and research with adult patients suggests that lithium also may be an effective treatment for comorbid substance dependence. However, no double-blind, placebo-controlled studies have tested the therapy in adolescents. Now, at Washington University in St. Louis, Dr. Barbara Geller and her colleagues have found that, in adolescent patients, lithium treatment for the manic phase of bipolar disorder also reduces drug and alcohol dependence.
The researchers' double-blind, placebo-controlled study involved 25 teenage patients who had been diagnosed with bipolar disorder and secondary substance abuse disorder involving marijuana, alcohol, inhalants, or multiple drugs. "Most of these kids have had bipolar disorder since the age of 9," Dr. Geller says. "They have been severely ill for a long time, and most are from families with a history of bipolar disorder."
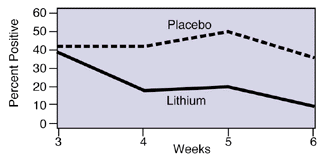 Percent of Urine Samples Positive for Drugs: Patients Taking Lithium vs. Patients Taking a Placebo. Random weekly urine analysis showed significantly lower drug use among patients who received lithium compared with patients who received a placebo.
Percent of Urine Samples Positive for Drugs: Patients Taking Lithium vs. Patients Taking a Placebo. Random weekly urine analysis showed significantly lower drug use among patients who received lithium compared with patients who received a placebo.More than half of the patients also came from families with a history of substance abuse, sometimes reaching back several generations. All had begun using drugs in the year prior to being enrolled in the study. "Secondary substance dependence disorders are the most common and most severe comorbidity in bipolar patients," Dr. Geller says. "We wanted to get to them within the first year, when they were newly addicted."
All participants in the study received packets of capsules to be taken twice each day during the 6-week study. For half the teenagers, the capsules contained lithium dosages that have proven effective in treating adult bipolar patients. The other patients received placebo only. All participants, who were treated as outpatients, also received weekly therapy sessions. Blood levels of lithium were checked twice each week - once randomly - to make sure the participants were taking the pills. Urine samples were collected twice weekly - once randomly - to monitor drug use.
The percentage of drug-positive urine samples for participants receiving placebo remained essentially unchanged, at roughly 40 percent, throughout the study. But for the group receiving lithium, drug-positive urine samples dropped from 40 percent to approximately 10 percent. "We tested randomly six times during the study and the urine samples confirmed the patients' self-reports. There was a significant decrease in drug use," Dr. Geller says.
In addition, patients in the lithium group showed significantly greater improvement in symptoms of bipolar disorder - such as their ability to function in family, school, and social settings - than did those receiving a placebo.
"Lithium treatment of bipolar disorder in adolescents with secondary substance dependence disorders was an efficacious treatment for both disorders," Dr. Geller concludes.
Reducing Craving in Methadone Patients
Dr. Edward Nunes and his colleagues at the New York State Psychiatric Institute and Columbia University College of Physicians and Surgeons in New York City found that antidepressants used to treat comorbid depressive disorders in adult methadone treatment patients not only can improve their mood but also reduce their craving for drugs.
"We were able to identify and treat primary or secondary depression in chronically drug-dependent adults," Dr. Nunes says. "In some respects, treating depression as a separable disorder represents a sea change in the way we look at comorbidity in these patients."
In Dr. Nunes' study, patients receiving imipramine to treat depression showed substantial drops in depressive symptoms, and many patients whose depressive symptoms improved also reported decreased craving and use of drugs, including opiates, cocaine, and marijuana.
"There is evidence that treating the depression helps some patients take advantage of therapy and could be successful as one part of treatment," Dr. Nunes says.
The 12-week study involved 137 patients recruited from 2 community-based methadone maintenance programs. Patients also were diagnosed with primary depression that predated their drug use or secondary depression that emerged or persisted through a period of abstinence or had lasted for at least 3 months during a current period of drug use. Patients were randomly assigned to either imipramine or placebo. Eighty-four patients completed at least 6 weeks of the trial. Fifty-seven percent of patients receiving imipramine were rated as having substantial improvement in both mood and drug use compared with only 7 percent among the patients receiving placebo. Fourteen percent of patients receiving imipramine achieved abstinence, confirmed by urinalysis, for 4 weeks compared with 2 percent of patients who received placebo.
"Imipramine had a very robust and positive effect on mood. This improved mood was associated with less intense and less frequent drug craving and, to a lesser extent, with reduced drug use," Dr. Nunes says.
Sources
- Geller, B., et al. Double-blind and placebo-controlled study of lithium for adolescent bipolar disorders with secondary substance dependency. Journal of the American Academy of Child and Adolescent Psychiatry 37(2):171-178, 1998.
- Nunes, E.V., et al. Imipramine treatment of opiate-dependent patients with depressive disorders. Archives of General Psychiatry 55:153-160, 1998.