The primary factor in the development of addiction is neurophysiologic reinforcement (reward). One specific mesolimbic "reward pathway" has been identified in the brain31, and others may exist. This pathway involves dopaminergic neurons that originate in the ventral tegmental area (VTA) and project into the forebrain, particularly the nucleus accumbens (See Figure 2 below). The dopaminergic neurons are probably under continuous inhibition in the VTA, perhaps by gamma-aminobutyric acid (GABA). Release of dopamine from these neurons onto the dopamine receptors in the nucleus accumbens produces positive reinforcement.
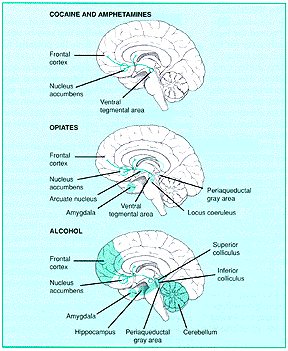 Animal studies suggest the existence of at least one central reward-reinforcement pathway for drug self-administration in the human brain. The stimulant-reward system (top) directly influences the neurons using dopamine that connect from the ventral tegmental area (VTA) to the nucleus accumbens (NA) and thereafter to the frontal cortex. The opioid system (middle) appears to involve structures such as the periaqueductal gray area, arcuate nucleus, amygdala and locus coeruleus, which use peptides that mimic the action of drugs such as heroin and morphine and indirectly influence the NA in a manner similar to that of stimulants. Alcohol and other sedative-hypnotics (bottom) also indirectly affect the VTA-NA reward system. This effect is mediated by GABA receptors, which are distributed widely and which influence the central dopaminergic reward system through mechanisms that include opioid pathways. (Adapted from Brain concepts: drugs and the brain. Washington, DC: Society for Neuroscience, 1992.)
Animal studies suggest the existence of at least one central reward-reinforcement pathway for drug self-administration in the human brain. The stimulant-reward system (top) directly influences the neurons using dopamine that connect from the ventral tegmental area (VTA) to the nucleus accumbens (NA) and thereafter to the frontal cortex. The opioid system (middle) appears to involve structures such as the periaqueductal gray area, arcuate nucleus, amygdala and locus coeruleus, which use peptides that mimic the action of drugs such as heroin and morphine and indirectly influence the NA in a manner similar to that of stimulants. Alcohol and other sedative-hypnotics (bottom) also indirectly affect the VTA-NA reward system. This effect is mediated by GABA receptors, which are distributed widely and which influence the central dopaminergic reward system through mechanisms that include opioid pathways. (Adapted from Brain concepts: drugs and the brain. Washington, DC: Society for Neuroscience, 1992.)Most stimulants - including cocaine, amphetamines and nicotine - exert their actions by elevating the synaptic levels of dopamine, norepinephrine and serotonin. Cocaine inhibits the monoamine reuptake mechanism, which is the primary mechanism for terminating transmitter action. Chronic cocaine self-administration appears to alter receptor sensitivities in the nucleus accumbens and other parts of the reward/reinforcement system32. Amphetamine stimulates the release of dopamine and norepinephrine and blocks their reuptake. Nicotine appears to exhibit its central effects through an interaction with nicotinic acetylcholine receptors that contain an integral transmembrane sodium channel33. Agonist binding leads to channel opening and depolarization responses.
Alcohol and sedatives such as the benzodiazepines and barbiturates are mood-altering drugs that depress the level of central nervous system arousal. They are believed to enhance the actions of the inhibitory neurotransmitter GABA, which are mediated by the GABAA receptor33. When GABA is released in the synaptic cleft, it binds to its receptor and opens chloride channels; this, in turn, hyperpolarizes the membranes, thereby lowering cell excitability. The long-term cellular changes engendered by this recurring process seem to interact with the reinforcement pathways through mechanisms that include the endogenous opioid systems, since craving for alcohol can be at least partially blocked by the opiate antagonist naltrexone (Trexan). Benzodiazepines and barbiturates also open the chloride channels through their actions at specific receptors. Ethanol does not appear to have a specific receptor, but it also interacts with the GABA A receptor complex.
The etiology of opioid addiction seems to involve at least some of the same final pathways (opioid systems to VTA to nucleus accumbens). Physical dependence and withdrawal syndromes are mediated by separate anatomical pathways and are now understood not to be a central feature of addiction. However, physical dependence and withdrawal syndromes are nonetheless clinically relevant and are related to changes in the reactivity of transmitter systems such as norepinephrine under tonic inhibition by endogenous opioid peptides or exogenous opiates. Thus, the opiate withdrawal syndrome includes a strong component of central adrenergic overflow. Physical dependence appears to be less of a problem with some drugs of abuse, including anabolic steroids, the cannabinoids, phencyclidine (PCP) and hallucinogens.
The potential for relapse in alcohol and drug addiction appears to persist indefinitely. The addicted person and the physician must be aware of this enduring risk. The acute craving may disappear after several weeks or months, but the relapse trigger may occur spontaneously at any time. Triggers may be purely internal or may be environmental, as in turning a corner and seeing a place or a person associated with addictive behavior in the past.