Dime-size arrays of tiny needles enabled volunteers to receive naltrexone via skin patch in a recent proof-of-concept clinical trial. If further work bears out the trial's success, the opiate antagonist and many other medications that are currently given orally or by injection may some day be administered by skin patch. In addition to avoiding painful needles and hard-to-swallow or stomach-irritating pills, transdermal delivery's advantages include well-controlled doses and steady medication blood levels over extended periods.
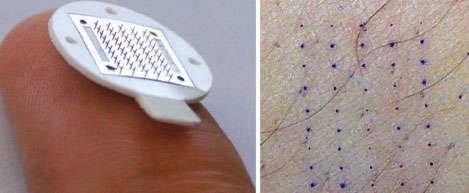 Tiny Needles Prepare Skin for Patch Medication: A microneedle array (left) is a small rectangle of 50 tiny needles, each 620 microns in length and thinner than a human hair. Tiny, painless epidermal punctures created by pressing the needles against the skin act as conduits for medication to flow evenly from a skin patch into dermal capillaries and the bloodstream.
Tiny Needles Prepare Skin for Patch Medication: A microneedle array (left) is a small rectangle of 50 tiny needles, each 620 microns in length and thinner than a human hair. Tiny, painless epidermal punctures created by pressing the needles against the skin act as conduits for medication to flow evenly from a skin patch into dermal capillaries and the bloodstream.Pharmaceutical researcher Dr. Audra Stinchcomb and clinical pharmacist Dr. Daniel Wermeling of the University of Kentucky and engineer Dr. Mark Prausnitz of the Georgia Institute of Technology developed the new technology. Pressed painlessly into the skin, their microneedles puncture the relatively impermeable outer layer of epidermis to create a grid of pores through which medication can readily and evenly pass from a skin patch to the skin's capillaries and into the bloodstream. The team opted to test the technology with naltrexone, a medication used to treat alcohol and opiate abuse, because current oral and injected methods of administering the opiate antagonist have drawbacks.
In the trial, a research assistant applied four arrays of microneedles to the upper-arm skin of six healthy volunteers for a few seconds. The participants reported that the arrays did not hurt and felt smooth against their skin. After removing the microneedles, the assistant fastened a naltrexone transdermal patch over the same area with small bandages.
Because transdermal medication does not pass through the digestive system before entering the bloodstream, it reaches target tissues without being exposed to degradation by liver enzymes. As a result:
- Therapeutic blood levels were achieved with 12.6 mg of naltrexone per day, which is only about a quarter of a typical oral dosage.
- The volunteers' blood naltrexone concentrations began to rise within minutes of the patch application, stabilized at an average of about 2.5 ng/mL within hours, and remained relatively constant for 2 days; after 72 hours, they had fallen by about half but were still in the range considered therapeutic. With oral medication, blood naltrexone levels take longer to rise and may fluctuate widely between doses, sometimes falling to levels that are therapeutically ineffective and sometimes spiking to levels that cause adverse effects.
- Naltrexone was converted to its primary metabolite, naltrexol, at a much slower rate than that measured with oral administration. Because high naltrexol levels have been correlated with adverse effects and patient dropout, keeping the levels low may enable more patients to tolerate naltrexone therapy.
The microneedle array was well-tolerated. Four patients developed redness and irritation at the site of the patch, which the researchers found to be due to the medication rather than the needles and which resolved during 2 weeks of antihistamine treatment.
The trial demonstration represents a first step toward medical use of micro- needles. The researchers next plan to look for a commercial partner and further refine the device.
"Many medications—those that are water-soluble, made of small molecules, or not easily absorbed orally—would be good candidates for microneedle-array delivery," says Dr. Wermeling. "The microneedle technology also opens up noninjection delivery for other therapeutic agents—including proteins, DNA, and vaccines—an advantage that is particularly exciting."
"Microneedle technology is part of a larger effort by NIDA-funded researchers to develop safer ways to deliver medications," says Dr. Moo Park of the Institute's Division of Pharmacotherapies and Medical Consequences of Drug Abuse. He notes that the new technology might increase patients' willingness to receive some important medical interventions, including vaccines. "Many patients avoid or are anxious about vaccine injections, and microneedle delivery of these important therapies has a promising future," he says. "The research is in the early stages but is an interesting area to watch."
Source
Wermeling, D.P. et al. Microneedles permit transdermal delivery of a skin-impermeant medication to humans. Proceedings of the National Academy of Sciences 105(6):2058-2063, 2008. [Full Text (PDF, 599KB)]