Offering voluntary HIV testing on a routine basis in outpatient health care settings would slow the spread of HIV and improve the survival of many of the estimated 280,000 Americans who are unaware that they are infected. The value of extending HIV screening to relatively low-risk populations in outpatient settings would be on par with the value of routine screening for other common conditions, such as colon cancer, according to two studies funded by NIDA.
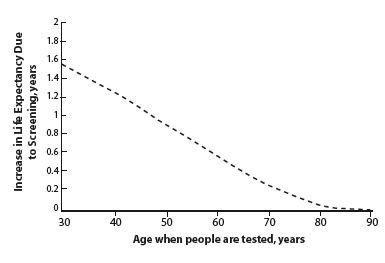 Study Predicts Routine Voluntary HIV Testing Would Extend Survival. Compared with HIV detection based on symptoms, routine voluntary HIV testing would enhance the life expectancy of people with the infection by getting them into life-prolonging care earlier. Estimates are based on the assumption that state-of-the-art therapy would be initiated when patients had a relatively favorable CD4 count of 350 cells/m3 as opposed to 175 cells/m3, the average count associated with detection based on symptoms. The CD4 count is a measure of immune system health.
Study Predicts Routine Voluntary HIV Testing Would Extend Survival. Compared with HIV detection based on symptoms, routine voluntary HIV testing would enhance the life expectancy of people with the infection by getting them into life-prolonging care earlier. Estimates are based on the assumption that state-of-the-art therapy would be initiated when patients had a relatively favorable CD4 count of 350 cells/m3 as opposed to 175 cells/m3, the average count associated with detection based on symptoms. The CD4 count is a measure of immune system health.In the United States, about one-quarter of the 1.04 million people estimated to be HIV infected do not know they have the virus. Under current testing guidelines, many of these individuals are likely to remain ignorant of their status for as long as they remain relatively healthy, because they do not belong to any of the high-prevalence subgroups to whom testing is recommended, and only those who live in areas with high infection rates will be screened as hospital inpatients. Meanwhile, their disease advances undiagnosed, compromising their prospects for future health and survival. They remain unaware of the need to take precautions against spreading the infection, and according to estimates from the Centers for Disease Control and Prevention (CDC), transmit the virus to 27,000 others each year.
Lead investigators in the two studies, Dr. A. David Paltiel of Yale University School of Medicine and Dr. Gillian Sanders of Duke University's Clinical Research Institute, used computer models to determine whether it would be cost-effective to extend routine voluntary screening to subpopulations with moderate prevalence of infection or to the whole population. The models use data on the estimated cost associated with an HIV test, the number of additional people who would be tested and the number of cases likely to be diagnosed sooner (and how much sooner), the greater benefits of therapy in earlier as opposed to later stages of infection, and the number of new infections that will be avoided when people who find out they are infected take precautions against transmission. Their work updates previous cost analyses by incorporating the use of state-of-the-art antiretroviral treatment (HAART) for HIV. The analyses yield estimates of the cost of each additional year of life expectancy that would be gained by expanded testing. Policymakers use such analyses to decide how to allocate funds for health.
Benefits of Early Detection
Dr. Sanders, Dr. Douglas Owens of the Veterans Affairs Palo Alto Health Care System, and their colleagues analyzed a hypothetical group of patients typical of those in general health care settings. The researchers assumed the patients' average age was 43 and their rate of unknown HIV infection was 1 percent, the level at which the CDC recommends routine testing. A 1 percent prevalence of unknown infection is probably high compared with the overall U.S. population (0.1 percent), but lower than high-risk populations currently screened (3 percent). By comparing three different scenarios of HIV detection—symptom-based diagnosis, a one-time voluntary test, testing every 5 years—the researchers were able to assess the lifetime benefits to patients and their partners, as well as the costs, of expanded testing.
The analysis found that one-time HIV testing would increase the life expectancies of individuals in the hypothetical population by an average of 4.7 quality-adjusted days and cost about $15,078 for every year of life gained. Patients whose HIV was discovered earlier and treated sooner would live on average 1.5 years longer as a result of the testing.
The $15,078 figure assumes that earlier HIV detection would reduce the spread of infection by 20 percent. Some such reduction would be likely because once people know they have HIV, they tend to change their behavior to avoid infecting others, and when they start antiretroviral treatment their fluids become less infectious. If transmission were not reduced, one-time HIV testing in the hypothetical population would cost $41,736 per year of life gained—comparable to the cost-effectiveness of routine testing for colon cancer, hypertension, and type 2 diabetes. The researchers further suggested that one-time testing might be justified in terms of value in a hypothetical population with an HIV infection prevalence as low as 0.05 percent.
In the second study, Dr. Paltiel and his colleagues compared current practice with routine voluntary HIV testing among high-risk communities (3 percent prevalence), communities with 1 percent prevalence, and the general population of the United States (0.1 percent prevalence). They estimated that adding a one-time voluntary HIV test to current care for people at high risk of infection would cost $36,000 per life-year gained. Testing a population that meets the 1 percent threshold raises the cost to $38,000—a figure similar to the $41,736 estimate of Dr. Sanders and colleagues. In the high-risk population, testing every 5 years would cost $50,000 per added life-year, rising to $63,000 if testing were done every 3 years. The findings suggest that voluntary testing every 3 to 5 years in all populations except those with the lowest prevalence would increase survival at a comparatively attractive cost by U.S. standards, says Dr. Paltiel. A one-time voluntary screening in the general population may also be cost-effective, but merits further investigation, he adds.
HIV Testing and Other Routine Tests: Cost-Effectiveness Compared
| Test | $/QALY* Gained |
|---|---|
| HIV test: All inpatients† | 38,600 |
| HIV test every 5 years: People at high risk (3% prevalence)† | 50,000 |
| HIV test one time (1% prevalence)‡ Individual benefit only Including benefit to others |
41,736 15,078 |
| HIV test one time: U.S. general population (0.1% prevalence)† | 113,000 |
| Breast cancer test: Annual mammogram, age 50-69§ | 57,500 |
| Colon cancer test: FOBT + SIG every 5 years, age 50-85§ | 57,700 |
| Type 2 diabetes test: Fasting blood glucose, age >25§ | 70,000 |
| Hypertension testing§ | 48,000 |
FOBT indicates fecal occult blood test; SIG, sigmoidoscopy.
*In quality-adjusted life years (QALYs), which account for both longevity and health-related quality of life. †Paltiel et al. (2005); ‡Sanders et al. (2005); §Adapted from personal communication, Sanders and Paltiel, 2005.
"Expanding voluntary HIV testing will require an investment—but it delivers better value for money than many other chronic disease testing programs that are routinely used in the United States today," says Dr. Paltiel. Neither research project addressed who should pay for expanded HIV screening, but the findings serve as a springboard for policy discussions involving all people with a stake in the decision. "Cost-effectiveness is just one consideration in policy decisions. Implementing expanded HIV testing also will require people believing it's an important use of limited resources," says Dr. Sanders.
The findings have made an impact in the state with the largest HIV caseload in the nation. Citing the research, the New York State Department of Health has revised its HIV guidelines, urging State health care providers to integrate routine testing into their medical care, use rapid HIV testing, and refer patients with positive test results to care, among other things.
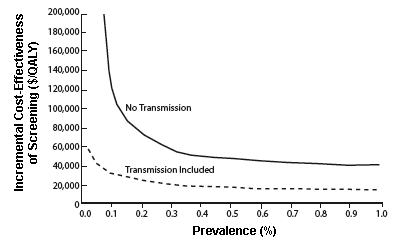 Study Estimates Range of Value Associated With Routine Voluntary HIV Testing. Dr. Sanders and colleagues estimated that routine HIV testing would be relatively economical even if the prevalence rates of undiagnosed infection were as low as 0.05 percent (half that of the U.S. general population estimate) when reduced transmission to partners is considered (dashed line). Even when transmission is not considered (solid line), HIV testing might be a financially attractive option at prevalence rates well below 1 percent.
Study Estimates Range of Value Associated With Routine Voluntary HIV Testing. Dr. Sanders and colleagues estimated that routine HIV testing would be relatively economical even if the prevalence rates of undiagnosed infection were as low as 0.05 percent (half that of the U.S. general population estimate) when reduced transmission to partners is considered (dashed line). Even when transmission is not considered (solid line), HIV testing might be a financially attractive option at prevalence rates well below 1 percent."People may think of computer-based analyses as isolated and abstract, but this AIDS modeling program encourages researchers to use findings from a wide range of relevant disciplines and incorporate advice from clinicians," says Dr. Peter Hartsock of NIDA's Division of Epidemiology, Services and Prevention Research. "These two studies integrated data from many perspectives, and their results provide rigorous but practical information that can guide the societal discussion of what to do about the problem."
Sources
- Paltiel, A.D., et al. Expanded screening for HIV in the United States—an analysis of cost-effectiveness. New England Journal of Medicine 352(6):586-595, 2005. [Abstract]
- Sanders, G.D., et al. Cost-effectiveness of screening for HIV in the era of highly active antiretroviral therapy. New England Journal of Medicine 352(6):570-585, 2005. [Abstract]